
Antimicrobial resistance (AMR) has been dubbed the silent pandemic over the past couple of years and this term is growing in popularity. According to the World Health Organization, “AMR occurs when bacteria, viruses, fungi, and parasites change over time and no longer respond to medicines making infections harder to treat and increasing the risk of disease spread, severe illness, and death”. Antimicrobials are used to treat infections and infestations in animals, humans, and plants; hence, they are a fundamental tool in our toolbelt to maintain the health of animals, humans, and plants. The United Nations Ad hoc Interagency Coordinating Group on Antimicrobial Resistance released a report in 2019 stating that “drug-resistant diseases could cause 10 million deaths each year by 2050 and damage to the economy as catastrophic as the 2008-2009 global financial crisis.” Currently, the number of global deaths is closer to 1 million, but if little is done to control this problem, that number will continue to climb.
Among the different groups of medicines against which pathogens have been developing resistance over the past years are antibiotics, probably the most widely known problem beyond the medical realm. Antibiotics in terrestrial and aquatic food-producing animals are used for growth promotion, treatment of disease, and prevention of disease spread or dand isease overall. In the European Union, as of 2006, the use of antibiotics as growth promoters is illegal, and, in the United States of America, as of 2017, the use of antibiotics important for human medicine as growth promoters is banned.
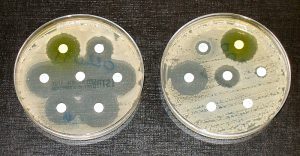
Antibiotic residues and antibiotic-resistant bacteria (ARB) are shed with animals’ excreta and can reach the environment and humans through direct and indirect pathways, depending on the production type and the treatment of waste. Terrestrial animal waste might reach water and soil around the farm due to animal movement, or, through run-off; it might also contaminate crops if used as manure or found in the irrigation water. Waste from aquaculture might disperse directly into the water and travel far with currents, an, travel far with currents, and wild animals, and enter into these pathways. Literature reviews and meta-analyses commissioned by the World Health Organization Advisory Group on Integrated Surveillance of Antimicrobial Resistance point to an important link between the use of antibiotics in animals and resistance arising in bacteria that infect both animals and humans.
The use of antibiotics in food-producing animals is to be framed by different practices aimed at preventing the development and spread of ARBs. These practices include steps that can reduce the need for antibiotics, such as vaccinations, and steps to use antibiotics sensibly and rationally. There have been some changes in the past months that apply to the latter. As of June 2023, antibiotics that are deemed as “medically important”, that is, antibiotics that are the same or like the ones used to treat diseases in humans, will no longer be sold over the counter, but will require a prescription from a veterinarian to be purchased or will be sold directly by veterinarians.
By: Olga Muñoz PhD | Graduate Assistant
 0
0
